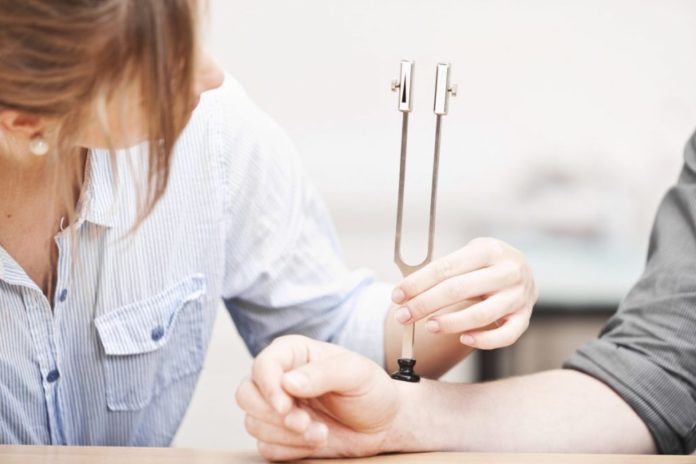
What is diabetic peripheral neuropathy?
Diabetic peripheral neuropathy is the most common form of peripheral neuropathy. A condition caused by long-term high blood sugar levels, in which nerves don’t work properly because they’re damaged or destroyed.
Uncontrolled high blood sugar can damage nerve fibers in your legs and feet. The condition usually develops slowly, sometimes for several decades.
Some people will not have any symptoms. But for others, symptoms may be debilitating. Symptoms include numbness or an inability to feel pain, a tingling or burning sensation, and itchiness. These are early symptoms of diabetic peripheral neuropathy.
Diabetic Peripheral Neuropathy affects the nerves in the hands and feet, causing sensations like:
• Numbness
• Tingling
• Pain
Nerve problems may also occur in your:
• Digestive tract
• Heart
• Eyes
• Other organ systems
What causes nerve damage?
Nerve damage is the result of high blood sugar levels sustained over a long period. It isn’t entirely clear why high sugar levels damage nerves.
Other factors can lead to nerve damage, such as:
• Low levels of insulin or treatment with insulin
• Damage to the blood vessels caused by high cholesterol levels
• Abnormal levels of vitamin B and vitamin E
• Lifestyle factors, such as smoking or alcohol use
• Side effects of certain medications, such as chemotherapy
• Trauma that causes pressure on nerves
• Mechanical injury, such as injuries caused by carpal tunnel syndrome
• Autoimmune diseases and infections
Diabetic peripheral neuropathy usually first appears in the feet and legs and may occur in the hands and arms later.
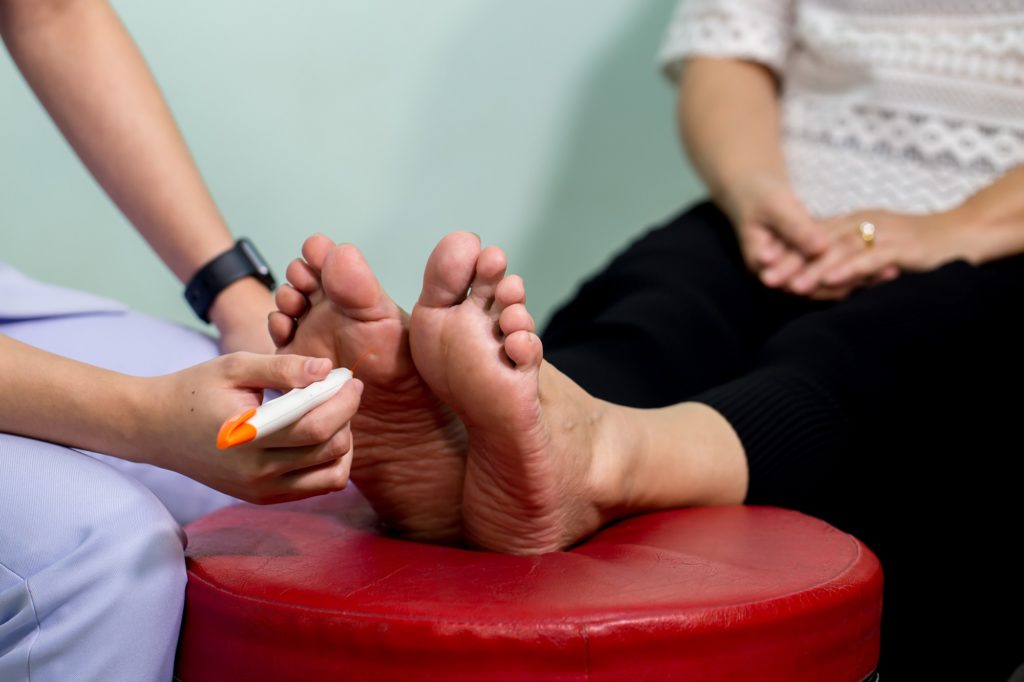
Diabetes affects the sensory, motor, and autonomic nervous systems. Your motor nerves send messages from the brain to the muscles so you can control your movements.
If the motor nervous system is damaged. Motor neuropathy symptoms might include:
• Muscle cramps
• Twitching
• Muscle weakness
• Foot drop
• Muscle wasting
• Paralysis
While your sensory nerves send messages from other body parts to the brain and trigger your senses. And if the sensory nervous system is damaged, symptoms might include:
• Prickling and tingling sensation, or “pins and needles”
• Numbness
• Reduced sensations of pain or hot and cold
• Increased pain from things that shouldn’t cause pain, like light touch
• Burning or sharp pain
• Loss of balance or coordination
Lastly, the autonomic nerves control involuntary and semi-voluntary functions including blood pressure, heart rate, bladder functions, and sweating.
If damaged, autonomic neuropathy symptoms include:
• Constipation or diarrhea
• Bloating, belching, or feeling of sickness
• Faint or dizziness upon standing from low blood pressure
• Rapid heart rate
• Sweating too much or too little
• Problems with sexual function
• Loss of bowel control
• Difficulty emptying the bladder completely
If those nerves were damaged by your diabetes, which is a complex web of nerves that connect the central nervous system to the rest of the body. This is the reason diabetic peripheral neuropathy can cause symptoms and complications just about anywhere on the body.
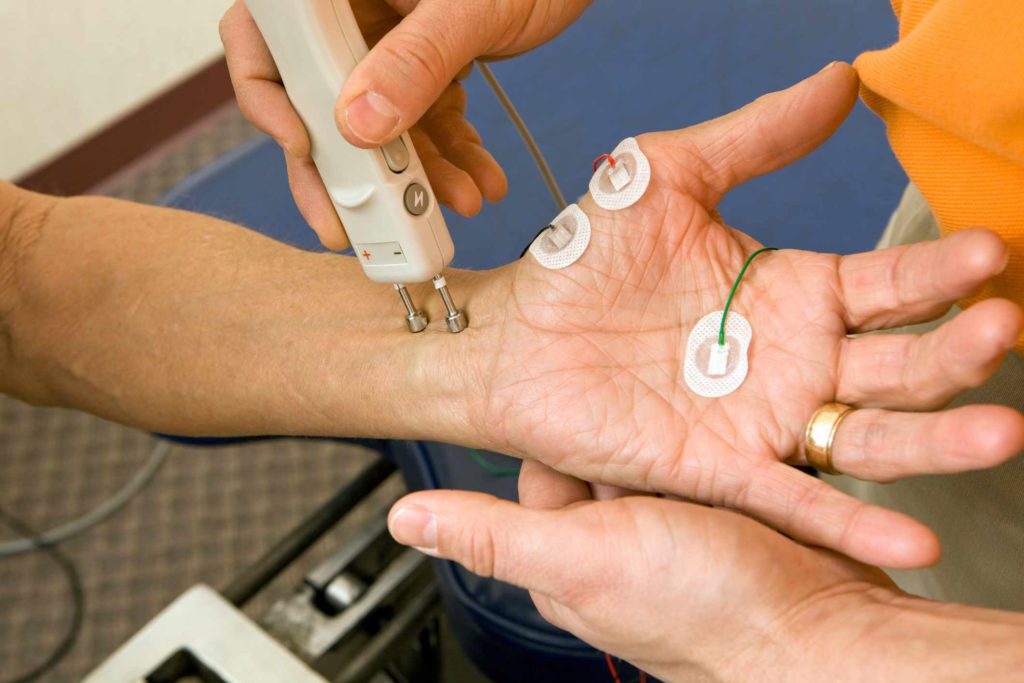
Feeling numbness
Diabetes damages the nerves. Diabetic peripheral neuropathy symptom is numbness or tingling in your extremities, including:
• Fingers
• Toes
• Hands
• Feet
You may also have a “pins-and-needles” feeling or even a burning sensation.
Shooting pain
You may experience sudden, sharp pains that feel like an electric shock. It is a result of damaged nerves that are sending out mistaken signals to the brain.
You may feel cramping, like when you’re grasping something like a piece of silverware. Sometimes you may unintentionally drop items you’re holding as a result of diabetic peripheral neuropathy.
The sensations may come and go but also remains constant at times. These pains mostly come at night and they can disturb your sleep.
Hot and cold
Exaggerated sensations happen when you have diabetic peripheral neuropathy. Your nerves help you sense everything around you. They are how you will notice when you are feeling hot or cold.
An example of this is, when holding a cup of warm coffee, you may feel painfully hot. Sometimes, you may hurt when a person with cold hands touches you. And your hands or feet may feel hot or cold for no apparent reason.
Foot problems
Losing function of the nerves in your feet, you might notice the following skin conditions at first until it becomes:
• Inflamed
• Infected
• Swollen
Doctors recommend that if you have diabetes, you check your feet and hands daily for injuries, especially if you’ve experienced nerve damage and lack of feeling in your fingers or toes.
Other common signs and symptoms of diabetic peripheral neuropathy
• Hypoglycemia (low blood sugar) symptoms, including shakiness, sweating, and a fast heartbeat
• Muscle wasting/sarcopenia
• Digestive problems, including bouts of constipation and diarrhea, nausea, vomiting, bloated stomach, and loss of appetite
• Low blood pressure, especially abruptly after standing up
• Loss of balance, dizziness, and fainting
• Sexual dysfunction, erectile dysfunction in men, and problems with vaginal lubrication and arousal in women
• Changes in perspiration, heavy night sweating, the inability to regulate internal temperature, or complete lack of perspiration (anhidrosis)
• Damage to the kidneys
• Damage to the nerves in the bladder and urinary tract, which cause frequent urination
Coping with nerve damage
Nerve damage from diabetes can’t be reversed. To avoid or limit any of these symptoms, it is important to manage your blood glucose. The more you can keep your levels in the normal range, it can help prevent additional damage to your nerves. You can better manage your blood glucose through the following methods:
• Avoid foods high in excess sugars, including sodas, sweetened drinks and coffees, fruit juices, and processed snacks, and candy bars.
• Eat foods high in fiber. These foods typically help keep blood sugars at a steady state.
• Eat foods that contain healthy fats, like those from olive oil and nuts, and choose lean proteins like chicken and turkey.
• Eat vegetables and plant-based proteins regularly, such as beans and tofu.
• Exercise at least five times a week, 30 minutes each time. Include aerobic activity and weight training in your routine.
• Monitor your blood sugar according to your doctor’s recommendation and record your levels. This will help you identify patterns and unusual changes in your blood sugar levels.
• Take insulin or oral medications, such as metformin (Glucophage), as instructed by your endocrinologist or primary care doctor.
In addition to managing your blood glucose levels, it’s important to pay attention to your feet and legs. Nerves in the legs and feet can be damaged, which can lead to reduced feeling. To prevent damage to your feet or legs:
• Regularly check your feet for open wounds or sores
• Clip your toenails
• Wash your feet with soap and water regularly
• Regularly visit a podiatrist
• Avoid walking barefoot
Talk to your doctor about lifestyle changes and tools that can help you cope if nerve damage has occurred.
Also, many treatments can help lessen the discomfort and pain caused by diabetic nerve pain, and your doctor can assist you in selecting one that works best for you.